Contact - Dr. Bennett's Veterinary House Calls - Allergic Skin Disease in Dogs in Contra Cost County, Wellness, General Veterinary Services.
Mobile Veterinarian In The East Bay Area California
- posted: Mar. 31, 2026
Allergic Skin Disease in Dogs in Contra Cost County
There is nothing normal about a persistently itchy pet. Allergic skin disease is one of the most common medical problems treated by veterinarians, and its impact is particularly noticeable in Northern California communities such as Contra Costa County. Unlike people who usually develop respiratory symptoms, pets primarily express allergic disease through the skin.
Dogs typically develop allergic skin disease from one of three sources: fleas or other insects, environmental allergens like pollen, mold, and dust mites, or food sensitivities. Flea allergies are by far the most common, with environmental allergies occurring next most often. Food allergies are less common but can still play a role in some pets.
While no formal county‑level prevalence studies exist for allergic skin disease in pets, regional and state‑level data strongly suggest that Contra Costa pets experience rates equal to—or higher than—national averages. Nationwide studies estimate that 10–15% of dogs are affected by allergic skin disease, with some populations reporting rates as high as 30%. In cats, dermatologic disease affects 6–15% of the general population, with allergic disease among the leading causes of chronic pruritus.
What Makes Contra Costa Different?
Several locally documented factors place pets in Contra Costa County at elevated risk for allergic skin disease:
- Climate and flea ecology: Northern California’s mild winters allow fleas to survive year‑round, eliminating the “off‑season” seen in colder regions. Flea allergy dermatitis is the most common allergic skin disease in dogs in the United States, and warm, temperate climates significantly increase the risk.
- Rising allergy trends in California: Pet insurance data show a 56% increase in allergy claims in California over recent years, with allergies now the top reason for veterinary visits statewide. Contra Costa County shares the same environmental exposures driving these trends.
- Urban–wildlife interface: Contra Costa’s mix of suburban development, open space, wildlife corridors, and indoor–outdoor pets create ideal conditions for persistent flea exposure, environmental allergens, and contact allergens—key contributors to chronic skin disease.
Why This Matters for Contra Costa Pet Owners
Pets in Contra Costa County are exposed to multiple overlapping allergy triggers—fleas, pollens, molds, dust mites, food allergens, and contact allergens—often simultaneously. Unlike people who usually develop respiratory symptoms, pets primarily express allergic disease through the skin. Without early intervention, chronic itching frequently leads to secondary bacterial or yeast infections, ear disease, and significant discomfort.
Recognizing allergic skin disease early and addressing it systematically allows veterinarians to interrupt the itch–infection cycle, reduce unnecessary treatments, and design a long‑term management plan that reflects the real environmental challenges faced by pets living in Contra Costa County.
Diagnosis and treatment of allergic skin disease
The first objective is to provide relief to the patient.
- Most veterinarians will use appropriate medications to stop inflammation and secondary infection
- The second objective is to educate the client about allergic skin disease
- Attempt to diagnose the cause of the allergic skin disease so that a permanent and long-term treatment plan can be employed.
Fleas and Allergic Skin Disease in Contra Costa County
Fleas are a leading cause of allergic skin disease in dogs and cats throughout Contra Costa County. When fleas bite, they inject saliva that can trigger intense itching and inflammation. In flea‑allergic pets, even one flea bite can cause severe symptoms, known as flea allergy dermatitis (FAD).
Importantly, itching severity does not reflect flea burden. Pets with flea allergies may react to a single bite, while others show minimal signs despite exposure.
Where Fleas Live: Home and Yard Infestations
Fleas primarily infest the environment—not the pet. Eggs and immature stages develop in carpets, bedding, furniture, crawl spaces, and shaded outdoor areas. Adult fleas emerge in response to heat and movement, then jump onto pets to feed.
Because of this life cycle, treating only the itchy pet is ineffective. All pets in the household must receive flea prevention.
Flea Control as a Diagnostic Step in Allergic Pets
For pets with chronic or seasonal itching, effective flea control is a required diagnostic step. Without eliminating fleas, other allergy treatments, including food trials and environmental management—may fail.
Successful flea control requires:
- Consistent flea prevention for all pets
- Environmental cleaning
- Addressing wildlife or rodent exposure when present
Choosing Effective Flea Prevention for Allergic Skin Disease
Topical Flea Control Products
Topical (contact‑kill) products remain on the skin and kill fleas on contact. Effectiveness varies widely. Some products—especially those containing permethrin—are toxic to cats and unsafe in mixed‑pet households.
✔️ Topical‑Only Insecticide Categories
|
Systemic Flea Medications
Systemic flea preventatives circulate internally and kill fleas after they bite. These products provide more consistent protection and are often preferred for pets with flea allergy dermatitis, particularly in high‑risk environments.
Category | Example Active Ingredients | How They Work | Notes |
Isoxazolines | Afoxolaner, Fluralaner, Sarolaner, Lotilaner | Systemic adulticides; kill fleas and ticks after they bite | Prescription‑only; long duration; highly effective |
Spinosyns (Systemic Oral) | Spinosad | Oral systemic adulticide; kills fleas after ingestion | Fast kill; cannot be used with high‑dose ivermectin |
Neonicotinoids (Oral) | Nitenpyram | Rapid systemic adulticide | Very short duration (24–48 hrs); used for quick knockdown |
Systemic IGRs | Lufenuron | Prevents flea eggs from hatching | No adulticidal activity; requires combination therapy |
Topical‑Systemic Macrocyclic Lactones | Selamectin, Moxidectin | Absorbed through skin → systemic | Kill fleas after feeding; also treat mites, heartworm, etc. |
Key Takeaways: Fleas and Pet Allergies
- Fleas are a common trigger and amplifier of allergic skin disease
- A single flea bite can cause significant itching
- Flea control is diagnostic, therapeutic, and preventative
- All pets must be treated for control to succeed
Effective allergy management in Contra Costa County starts with reliable, year‑round flea control tailored to your pet and home environment.
Food Allergy in Dogs
Food allergies are the least common cause of allergic skin disease in dogs, but it is still an important factor to rule out in pets with chronic itching. The most common food allergens are animal proteins, such as beef, chicken, fish, and lamb. Carbohydrates like rice or potatoes are rarely the cause of true food allergies.
Because effective flea control is always the first step, veterinarians often recommend a prescription food trial as the next diagnostic step. This involves feeding a specially formulated hypoallergenic diet for 6–8 weeks, with no other treats, table food, or flavored supplements during the trial.
Food allergies in dogs are typically year‑round, either acting alone or in combination with other allergies. In Contra Costa County and other Northern California climates, fleas can also be present year‑round, which is why flea allergies must be ruled out before starting a food trial. Your veterinarian will help determine whether food allergies are contributing to your pet’s skin condition and guide you through the process.
Atopy (Environmental Skin Allergies)
Atopy refers to allergic skin disease caused by environmental allergens such as pollen, molds, and dust mites. These allergens are either inhaled or come into contact with a pet’s skin, triggering an allergic reaction. In dogs, atopy is a diagnosis of exclusion, meaning it is typically presumed after flea allergy and food allergy have been ruled out.
Once a presumptive diagnosis of atopy is made, there are two primary treatment approaches.
Treatment Option 1: Allergy Testing and Immunotherapy
Allergy testing can be performed to identify specific environmental allergens that may be triggering a dog’s symptoms. This may be done through a blood test or intradermal skin testing, in which a small area of the pet’s skin is shaved and tiny amounts of suspected allergens are introduced and monitored for a reaction.
If relevant allergens are identified, allergen‑specific immunotherapy (“allergy shots”) may be recommended. These injections are given regularly over time, and approximately 60–70% of dogs experience partial or significant improvement. Immunotherapy is considered a long‑term management strategy rather than a cure.
Pros and Cons of Allergy Testing and Immunotherapy
While immunotherapy can be helpful for some dogs, there are important limitations to consider. Environmental allergens are increasingly difficult to predict due to the widespread use of non‑native ornamental plants, especially in regions like Contra Costa County and Northern California. Testing and treatment can also be costly, require long‑term commitment, and must be continued indefinitely to maintain results. In addition, adverse reactions—ranging from mild injection‑site swelling to rare but serious anaphylactic reactions—can occur.
Treatment Option 2: Medical Management
The most common and practical approach to treating atopy is medical management using immune‑modulating medications. These drugs reduce the immune system’s overreaction to allergens and help control itching and inflammation. Common categories include corticosteroids (immunosuppressive), Calcineurin inhibitor (immune modulator with potential immunosuppressive activity), Janus kinase inhibitors (immune modulator), Interleukin monoclonal antibody injections (immune modulator).
Immune Modulation vs. Immunosuppression — Explained Simply
Some allergy medications work by modulating the immune system rather than suppressing it. Immune modulation means calming an overactive allergic response while allowing the immune system to continue performing its normal protective functions. This targeted approach focuses on specific allergy pathways that cause itching and inflammation.
Immunosuppression, in contrast, broadly reduces immune activity. While this can be useful in certain diseases, it may also lower the body’s ability to fight infections when used long term.
Many modern treatments for allergic skin disease such as Apoquel®, Cytopoint®, and cyclosporine—are designed to modulate specific immune signals involved in allergies, rather than shutting down the immune system as a whole. This allows effective itch and inflammation control while maintaining overall immune health.
Medical therapy is often combined with topical treatments, such as medicated shampoos, sprays, or creams, to reduce inflammation, remove allergens from the skin, and control secondary infections. In some cases, systemic antibiotics or antifungal medications may be used at the beginning of treatment if infection is present.
This approach is widely used because it is effective, flexible, and easier to manage for most pets and families. Your veterinarian will tailor the treatment plan to your dog’s needs and discuss how each medication works, potential side effects, and long‑term expectations.
In some cases, itching and self‑injury aren’t caused by allergies at all. Conditions such as mites, infections, immune‑related disease, or other medical problems can look very similar at first. That’s why recognizing patterns early is so important. The sooner a veterinarian can identify what’s really causing the itch, the sooner we can break the itch–infection cycle and create a treatment plan that works for both the pet and the family. It’s common for owners to make reasonable guesses about why a pet is itching, but those assumptions can sometimes lead to wasted time and frustration. A step‑by‑step, medical approach helps us pinpoint the true cause and move toward lasting relief
In conclusion, no pet should live a life of misery due to painful and pruritic skin. Please call Dr. Bennett’s Veterinary House Calls if your pet is suffering due to skin problems.
Written by David Bennett, DVM
© 2026 [Dr. Bennett’s Veterinary House Calls]. All rights reserved.
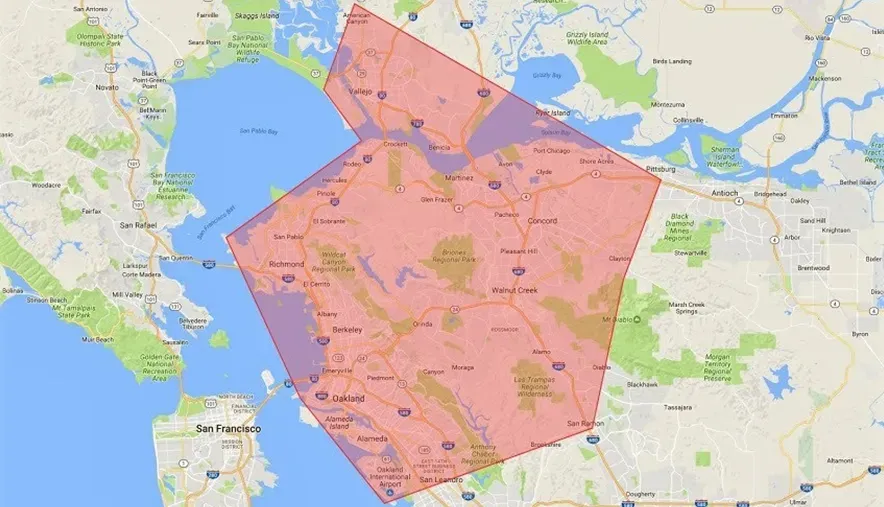
Territory Of Service
Dr. Bennett’s Mobile Veterinary Service provides compassionate in‑home pet euthanasia, outpatient medical care, and wellness services throughout Contra Costa County. Our central location near El Sobrante allows us to reach families across the East Bay, including Walnut Creek, Orinda, Moraga, Lafayette, Pleasant Hill, Martinez, Hercules, Pinole, El Sobrante, Richmond, Kensington, and Albany, as well as nearby areas such as Alamo and Danville.
Location
Find us on the map
Dr. Bennett's Veterinary House Calls
East Bay Mobile Veterinarian
Walnut Creek, CA 94598, US
510-964-2000

